Among the many camps of ideas for how to increase access to justice, one of the strongest I keep returning to is Devolved Legal Services. What I mean by this:
How can we devolve legal services out of offices — out of legal bureaucracies — and into community spaces?
How can we integrate legal help into other (often, more trusted & more accessible) organizations & institutions, so that a person can get easier access to legal professionals — as well as a more holistic solution to their problem?
Legal help may be devolved into schools, into libraries, into places of worships — and into hospitals. Medical-legal partnerships are one of the most established forms of devolved legal services.
The Milken Institute School of Public Health at George Washington University has established a National Center for Medical-Legal Partnership, that provides information on the health centers & legal organizations that have made such partnerships — as well as best practices & a starter toolkit for those interested in opening a partnership (you just have to complete a short form on their site to download the toolkit).

Such a partnership can take many forms: with lawyers physically stationed inside emergency rooms, clinics, or hospital wards — or with the medical organization having established a channel to lawyers, to funnel certain clients to them for consultations & help.
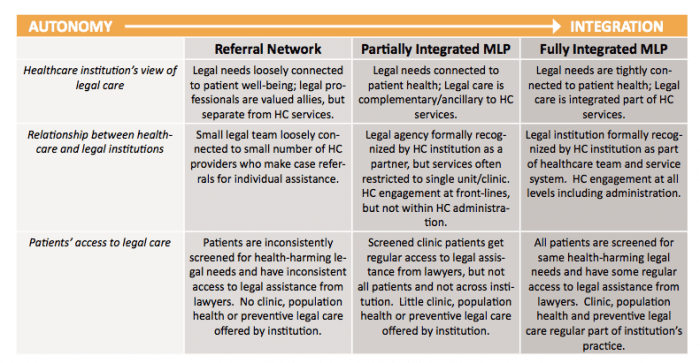
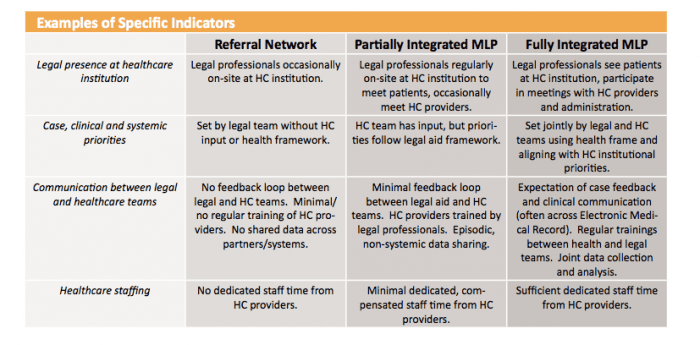
This new universe of medical-legal partnerships is a great example of how other community touchpoints can be made into legal ones. It also shows fruitful collaborations between other professionals and legal ones, to give a fuller & more satisfying service to the end-user.
As the National Center’s toolkit suggests — there is a huge crossover of medical problems & legal ones, but the two camps of professionals do not speak to each other — or if they do, they do not speak the same language. A structured partnership can uncover these links & build new service models, that benefit the individual end-user in the short-run and the community in the long-run, by enforcing the laws in a more systematic way that will stop bad practices that lead to health & legal problems.
The toolkit addresses the medical professional’s mental model, trying to expand it to include legal services.
Legal needs are not currently part of the language of healthcare, nor is legal care a tool in the toolbox healthcare team members use to treat patients or address population health. The connection between legal needs and health is invisible in the provision of healthcare. Overcoming this invisibility will require considerable education, not just about the connection between legal needs and health, but also about how lawyers can help each member of the healthcare team provide the necessary care. Medical-legal partnership builds on an existing framework, asking healthcare team members to expand their understanding of social determinants of health to recognize that some of those problems require legal screening and intervention. It asks them to accept lawyers – as they have patient navigators, case managers and social workers – as unique but indispensable members of the healthcare team with a new expertise to help identify, treat and prevent these problems in patients, clinics and populations.
It also tries to stretch legal professionals’ service models, to start thinking outside of traditional ways of problem-solving and client-service.
Legal institutions already provide assistance to individuals around many issues that impact health, but do so in a justice-driven framework, not a health-driven one. Medical-legal partnership requires legal institutions and professionals to dramatically re-orient the delivery of legal aid to prioritize health and to practice law in a public health framework, valuing population outcomes alongside individual case outcomes. Lawyers learn from their healthcare partners how to evaluate their work and adopt health-related priorities. It also asks legal professionals to move from crisis driven care (justice is about righting a wrong) to practicing prevention and upstream care. Legal services provided still include traditional typical case representation, but significantly shift time and resources to training healthcare team members and collaborating with healthcare team members on clinic and population health changes.
For some case studies of partnerships in action, here is a recent article from Tina Rosenberg at The New York Times that profiles some such partnerships in action in Cincinnati, Boston & New York
When Poverty Makes You Sick, a Lawyer Can Be the Cure
By TINA ROSENBERG July 17, 2014 9:30 pm
By early summer 2010, the temperature had already reached 100 degrees in Cincinnati. At Cincinnati Children’s Hospital Medical Center, doctors were urging the families of children with asthma to use air-conditioning. One mother handed a piece of paper to her doctor: The child’s room did have a window unit, and she was using it. But then the landlord responded — he apparently didn’t want to pay the electric bills. Use that air-conditioner, the letter said, and you will be evicted.
A concerned doctor might have tried to call the landlord to fight the notice. Or, she might have handed the letter over to a social worker. But Cincinnati Children’s had something better — it had lawyers. In 2008, the hospital and the Legal Aid Society of Greater Cincinnati set up a medical-legal partnership, the Cincinnati Child Health-Law Partnership or Child HeLP.
A week later, another family came in with the same letter. And the week after that.
“Our lawyers were getting the same problem referred over and over in a short period of time,” said Elaine Fink, who is the co-leader of Child HeLP. “They looked at the map — they were all in the same neighborhood. They looked to see who owned the buildings. In this case we hit bingo — the same owner.”
That was the Brooklyn-based NY Group, which held 18 buildings in Cincinnati and one in Dayton. Many tenants in those buildings had ended up at Child HeLP — to get help with mold, water damage, structural perils, rodents or bug infestations.Child HeLP wrote to NY Group, including in its letters statements by physicians about the health impacts of its legal violations. It sued on behalf of one severely disabled boy with a tracheotomy whose health depended on air-conditioning. The repairs were done in a few weeks.
But the point was not just to help individual patients — it was to improve conditions in the buildings for all tenants. At the same time, NY Group was walking away from the buildings — Fannie Mae foreclosed on all 19 by the end of July. Legal Aid helped tenants to organize and have a voice in the foreclosure process — among other things, they wanted to make sure that the buildings remain subsidized housing.
Ultimately that pressure resulted in widespread repairs, and helped persuade Fannie Mae to sell the buildings to Community Builders, a Boston-based nonprofit that develops and operates good low-income housing (which is maintaining the subsidies). Reconstruction is about to start.
Being poor can make you sick. Where you work, the air you breathe, the state of your housing, what you eat, your levels of stress and your vulnerability to crime, injury and discrimination all affect your health. These social determinants of health lie outside the reach of doctors and nurses.
In the early 1990s, Barry Zuckerman, the chief of pediatrics at Boston City Hospital (now Boston Medical Center), decided he was tired of seeing kids cycling back into the hospital again and again — asthmatic kids who never got better because of the mold in their houses, infants with breathing problems because their apartments were unheated. He’d write letters to the landlord, who ignored them, said Megan Sandel, who was an intern there at the time. Then at a cocktail party, someone listening to his complaints asked Zuckerman: What does the law say?
Zuckerman thought it was an important question. In 1993, he established the Family Advocacy Program with three lawyers to prod landlords, secure government benefits families were entitled to and fight with Medicaid, insurance companies, schools and other bureaucracies.
(Zuckerman deserves his own wing in medicine’s hall of innovation — he also co-founded Reach Out and Read, which supplies books and encourages doctors to prescribe them and family reading for kids. And he is co-founder of Health Leads, a program that trains college students to connect patients to food, heat and other basics of health.)
There were few medical-legal partnerships until about five or 10 years ago, but now 231 health care institutions have them, according to the National Center for Medical-Legal Partnership. The largest is New York’s LegalHealth, which works in about 20 New York hospitals and is expanding — it will soon have clinics in all 11 of the city’s public hospitals.
Medical-legal partnerships are growing in part because of increasing attention to social determinants of health. Talking about inequality means talking about the vicious cycles that keep people poor; one of the most important is the intersection of poverty and health. “And sometimes a new asthma inhaler isn’t going to solve the problem,” said Martha Bergmark, executive director of Voices for Civil Justice, and until recently director of the Mississippi Center for Justice.
The vast majority of low-income Americans have unresolved legal problems: debt, immigration status, custody issues, child care, benefits, back pay, housing, a special education plan for a child — you name it. All of these affect stress levels, which is in itself a health issue, but many have a more direct connection to health.
Medicaid in New York State is now, in some cases, paying for supportive housing. (Medicaid has long bought housing in the form of nursing homes, of course.) This WNYC radio story describes one formerly homeless woman now in a Medicaid-paid apartment. “You could treat her epilepsy until the cows come home, but without an appropriate place to live she was going to be sick,” said Bergmark.
Clinics that have medical-legal partnerships approach health differently than others. When doctors have no options for helping patients with the social determinants of health, they tend not to ask about them. With a medical-legal partnership, they do. At Cincinnati Children’s, each patient’s family is asked: Do you have housing problems? Problems getting your benefits? Are you depressed? Are you unsafe in your relationship? Would you like to speak to a lawyer or social worker about any of these things?
That process can start right away. “We have attorneys and paralegals on site in the primary care center five days a week,” said Fink. “Many times we get a legal aid attorney to walk down the hall to talk to family while the child is waiting to get immunizations.”
A legal letter can often get a response where a doctor’s or social worker’s letter does not. The lawyers also save doctors time. “Everyone works at the top of their profession instead of the physician figuring out why mom is going to be evicted tomorrow and what they can do about it,” said Ellen Lawton, co-principal investigator at the National Center for Medical-Legal Partnership.
The reverse is also true: adding doctors makes legal work easier. Lawton said that lawyers’ arguments carry more weight when they include a medical opinion. “The health of the kids changes the advocacy conversation,” she said. “It goes from ‘this is the law and you have to comply’ to a conversation that’s about community well-being and health. And when you’re able to use the clinical viewpoint rather than a legal framework, you’re able to resolve the issue much more rapidly.”
Most important, a medical-legal partnership goes beyond curing an individual. Child HeLP’s actions in Cincinnati’s sick buildings made life better for all the families there. “Don’t wait for the kids to be sick,” said Sandel, who is now the medical director of the national medical-legal partnership center. “Look for the pattern and find what’s making kids sick in the first place. The power of the model is moving upstream, going from person to person to population level” — legal action as preventive medicine.
Like other forms of preventive care, medical-legal clinics are a bargain. One striking example: New York City’s LegalHealth wrote formal legal demand letters to help adult asthma patients get their apartments cleared of rodents, bugs, mold, water and structural damage. The apartments were fixed. Patients improved, drastically, and there was a 90 percent drop in emergency room visits and hospital admissions. This was achieved by a one-shot intervention that cost an average of $225 per case.
But while society may save money, that’s not necessarily true for hospitals — and it’s hospitals that make the decisions. Fee-for-service medicine rewards hospitals for more admissions and emergency room usage, not less, and doesn’t reimburse hospitals for preventive services such as legal aid. Nor can legal aid lawyers rely on funding from the federal Legal Services Corporation, which never recovered from the Reagan administration’s cuts.
Increasingly, though, hospitals are establishing and paying for medical-legal partnerships, despite the lack of reimbursement. (New York City’s Health and Hospitals Corporation is paying for part of the expansion of LegalHealth, with other major funding from the Robin Hood Foundation, an anti-poverty group.) One reason is the growing move toward value-based reimbursement instead of fee-for-service — for example, Medicare now rewards hospitals for having low rates of readmission and good scores on safety measures. Nonmedical staff members such as social workers — and lawyers — are becoming a better investment.
Kerry J. Rodabaugh, a gynecologic oncologist at the University of Nebraska Medical Center, started a medical-legal partnership at an earlier job at the Roswell Cancer Center in Buffalo. She studied how often lawyers were able to get patients into insurance or benefit programs, which allows hospitals to be reimbursed for their care. She wrote a paper on the partnership’s work and the savings.
At Nebraska, Rodabaugh established a medical-legal partnership in her department.
“In order to get funding for my program I’ve had to prove a financial benefit,” she said. “I’ve been able to document at my current program a 700 percent return on investment since 2009. When I’m talking to administrators they get very excited.” Now U.N.M.C. is expanding these clinics to every department and to its primary care clinics in places with significant poverty.
“So much of child health is the result of poor social and physical living conditions for kids — food on the table, shelter, quality education,” said Robert S. Kahn, a pediatrician at Cincinnati Children’s who is the medical co-leader of Child HeLP. “So much of what we do in pediatrics is driven by these broader well-being issues for the family. We do much better when we partner with groups that have that as a mission.”
Join Fixes on Facebook and follow updates on twitter.com/nytimesfixes.
Tina Rosenberg won a Pulitzer Prize for her book “The Haunted Land: Facing Europe’s Ghosts After Communism.” She is a former editorial writer for The Times and the author, most recently, of “Join the Club: How Peer Pressure Can Transform the World” and the World War II spy story e-book “D for Deception.”